  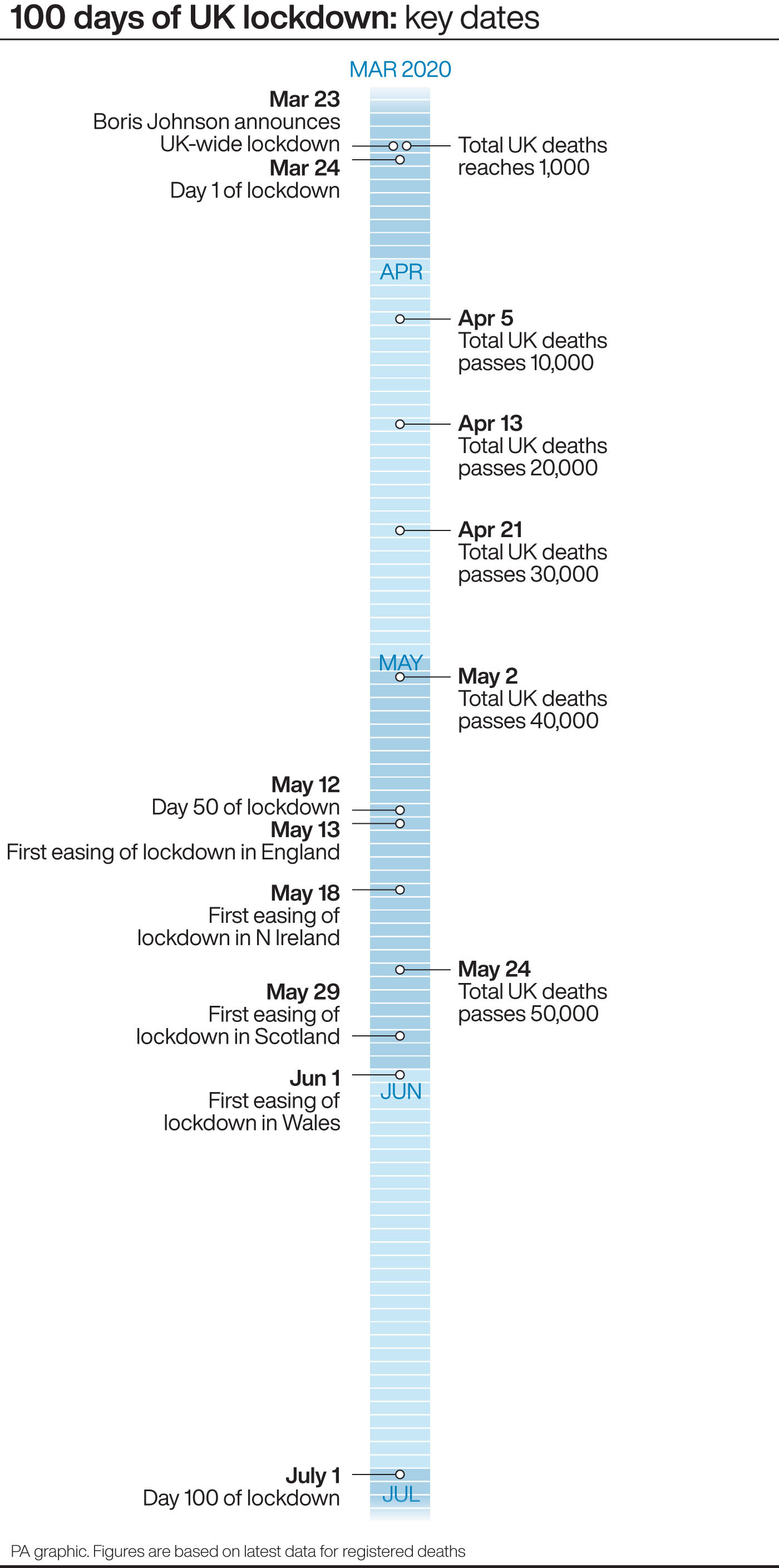
By March 26, 2020, when cases neared 927 and deaths were zero, the government announced a three-week national lockdown. 
By March 16, 2020, when the total reported cases had reached 64, South Africa declared a national disaster, banned travel from the worst-affected countries and public gatherings, and closed schools. However, the timing and intensity of those measures varied between countries. African countries’ success in containing and delaying the first wave of SARS-CoV-2 infections was partially attributed to the prompt and early introduction of NPIs. In the absence of effective pharmaceutical interventions early in the pandemic, non-pharmaceutical interventions (NPIs), or public health and social measures, were adopted to limit transmission and person-to-person contacts. While some countries have reported more infections than others, with South Africa, Morocco, Tunisia, Ethiopia, Egypt, Libya, Kenya and Zambia accounting for nearly 70% of all COVID-19 cases in Africa by Janu, the relatively low burden of COVID-19 in Africa compared to Europe and North America has been, in part, attributed to demographic factors such as younger and more rurally located populations, differences in case and death detection capacity, and environmental factors such as higher temperatures, as well as countries’ previous experience with outbreak prone diseases. With the first case on the African continent reported in Egypt on Febru, Africa accounts for 3.4 and 4.2% of measured COVID-19 cases and deaths, respectively. Over 352 million cases and 5.6 million deaths from coronavirus disease (COVID-19) have been recorded worldwide as of Janu. These data may be useful to understand transmission patterns, model infection transmission, and for pandemic planning. Increased stringency and decreased mobility were associated with a reduction in the number of contacts. We find a high reported number of daily contacts in all countries and substantial variations in mean contacts across countries and by gender. These are the first COVID-19 social contact data collected for 16 of the 19 countries surveyed. Mean contacts were correlated with Google mobility (coefficient 0.57, p=0.051 and coefficient 0.28, p=0.291 in August 2020 and February 2021, respectively) and Stringency Index (coefficient −0.12, p = 0.304 and coefficient −0.33, p=0.005 in August 2020 and February 2021, respectively). There were no strong and consistent variations in the number of mean or median contacts by education level, self-reported health, perceived self-reported risk of infection, vaccine acceptance, mask ownership, and perceived risk of COVID-19 to health. Men had more contacts than women and contacts were consistent across urban or rural settings (except in Cameroon and Kenya, where urban respondents had more contacts than rural ones, and in Senegal and Zambia, where the opposite was the case). Mean contacts increased for Ethiopia, Ghana, Liberia, Nigeria, Sudan, and Uganda and decreased for Cameroon, the Democratic Republic of Congo (DRC), and Tunisia between the two time points. Contacts of people aged 18–55 represented 50% of total contacts, with most contacts in household and work or study settings for both surveys. Mean reported contacts varied across countries with the lowest reported in Ethiopia (9, SD=16, median = 4, IQR = 8) in August 2020 and the highest in Sudan (50, SD=53, median = 33, IQR = 40) in February 2021. We described mean and median contacts across these characteristics and related contacts to Google Mobility reports and the Oxford Government Response Stringency Index for each country at the two time points. Adult respondents reported contacts made in the previous day by age group, demographic characteristics, and their attitudes towards COVID-19. We analysed nationally representative cross-sectional survey data from 19 African Union Member States, collected by the Partnership for Evidence-based Responses to COVID-19 (PERC) via telephone interviews at two time points (August 2020 and February 2021). However, few contact studies have been conducted in Africa. Social contact studies help measure the effectiveness of NPIs and estimate parameters for modelling SARS-CoV-2 transmission. Early in the COVID-19 pandemic, countries adopted non-pharmaceutical interventions (NPIs) such as lockdowns to limit SARS-CoV-2 transmission. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
